
Revenue Cycle Management
What is revenue cycle management? Is it the same as medical billing? Effective financial management is more than taking your fee ticket and creating a claim and sending it to the health plan or payer. It is called a “cycle” because success at each stage requires perfection at the stage preceding it. The revenue cycle for a medical practice includes multiple functions that must be performed at optimal levels by all involved physicians, managers, and staff:
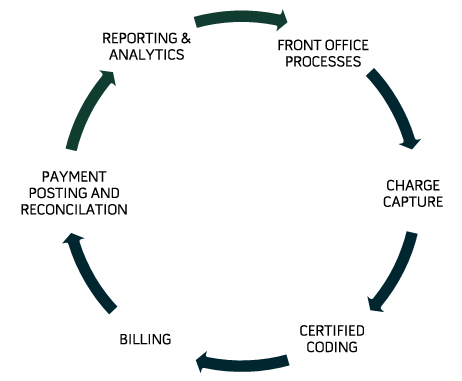
Front Office Processes
The revenue cycle begins with examining and improving your front office processes. How you collect patient insurance and demographic information and verify eligibility is critical. Get that wrong, and you will never receive payment for your services.
Charge Capture
The next critical step is how you capture charges – or “charge capture." Superbill? Electronic Health Record / Electronic Medical Record? Notecards? PDA? There is no right or wrong way. It is your system.
However you document your services, those charges must be captured if they are to be billed.
Coding
This is often the challenging part for medical practices. CPT, ICD-9, HCPCS, Modifiers – it is an acronym soup that is constantly changing. It takes experts to code right, the first time, and in compliance with the law. The New Directions team includes certified coders that spend much of their time learning and relearning new coding information. You should be paid for the right service and have peace of mind that the coding is done right.
Billing
Submitting your claim form to the correct health plan or payer daily starts the clock ticking on your receivables. How many days from the time you took care of a patient (“date of service”) is the bill sent out the door? And is it sent to the right payer? We get this right – all the time.
Payment Posting and Reconciliation
We make sure you receive payment for your services, by following up frequently with the health plan or payer. We will also make sure that the payment you receive is the correct one. We keep track of changes in CPT codes and reimbursement schedules, and any line items that have been denied. We get to know the payers and the representatives on a first name basis, so that they take good care of our clients.
Reporting and Analytics
Data, data, data. Information is power. In-depth reporting gives us insight into your practice and reimbursement trends by payer. We look for trends and respond quickly to them. Reports developed for you are easy to understand and give you the information at your fingertips. Need more information? We will be happy to create a report for you.